We are all made differently. We store body fat differently, we have different body frames and even different shapes. No one fitness model suits everyone. However, some concepts and theories apply to all human bodies since our bodies share a common evolutionary history.
While we know widely about Basal Metabolic Rate (BMR), which applies to our body functions in diverse forms and impacts our body weight, one of the least discussed theories is the Set Weight Point and its impact on an individual’s weight loss journey.
If you have ever been on a weight loss journey, there is a high chance that you have come across a plateau where your weight will not drop below a certain point for a long period. No matter how hard you try, changing your workout or deepening the calorie deficit, the weight just will not drop. Activities feel heavier, hunger spikes, concentration dips and with a sense of depreciating quality of life, you may halt your journey and witness a fast weight rebound. While you may think this is a lack of willpower or discipline, it is simply biology. You might have dropped below your Set Weight Point and now the brain is alarmed that you are in a survival crisis, even though you are practically not.
What most fitness cultures will not tell you is that your set point is biologically defended, i.e. your brain would not like your body to drop lower than that range and will use all internal mechanisms to store enough food- fat. The brain treats fat loss as dangerous and fat gain as relatively safe because, for millions of years of evolution, food scarcity was the dominant threat to survival. According to the settling point theory and set point theory (Keesey & Powley, 1986), the body treats its fat stores as a regulated biological system, not a passive reservoir. But that does not necessarily mean that the excessive fat reserves are necessary for you. It is simply what your brain has been told by your hormones for years.
What is a set weight point?
Our body defends a specific weight range, say for example 70-75kgs. About 5 to 10 pounds within this range our body feels “safe” and works to stay. This range is called the set point. It is not a single number on the scale. It is a range that your body actively fights to return to whenever you deviate from it.
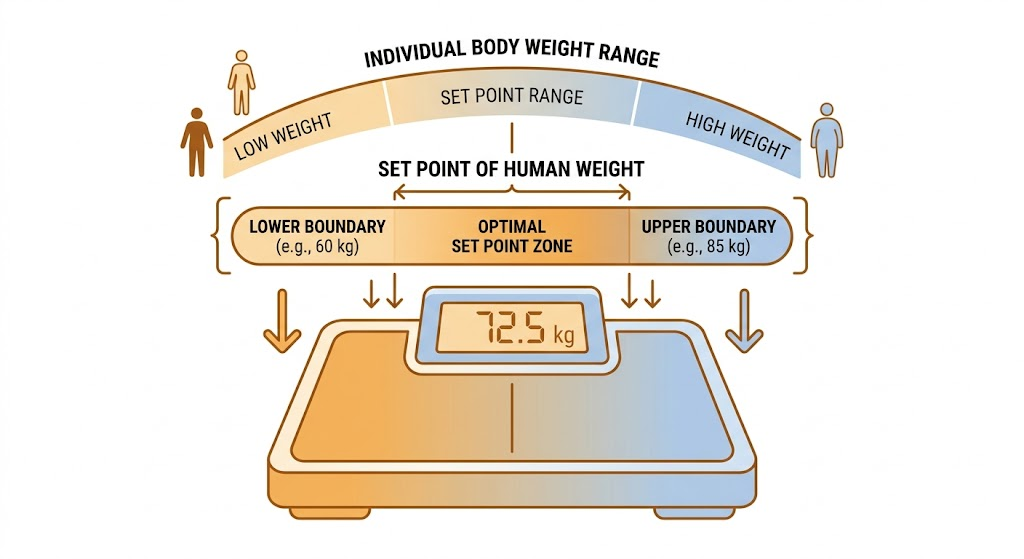
The set weight point is a composite output of several biological and environmental variables working together. It is different for different individuals, but everyone has their own set weight point. The arcuate nucleus inside the hypothalamus in our brain regulates this through a network of hormonal signals from the gut, fat tissue, and blood. According to the received signal, the brain adjusts hunger, metabolism, and behaviour, as it feels is necessary to defend its set weight.
Three major hormones carry those signals:
- Leptin– this hormone is released from fat cells. It informs the brain, “We have enough energy stored.” When fat mass drops, leptin drops. This becomes a starvation signal. It does not matter how much you consciously want to lose weight. The brain treats falling leptin like a life-threatening emergency.
- Ghrelin– this hormone from the stomach lining drives you toward food. It signals the brain when it’s time to eat food by triggering hunger. In a calorie deficit, ghrelin levels rise chronically because you are not satiating the hunger as before. It remains elevated even when you are not hungry by normal standards. Despite weight loss, ghrelin may take more than a year to drop to a more weight-appropriate level, and you stay hungrier in your weight loss journey.
- Insulin– this hormone tells the brain about blood sugar levels. Elevated insulin, from frequent high-carbohydrate eating, interferes with leptin signalling and enables higher fat storage because it makes the brain think that the body has less energy than it actually does.
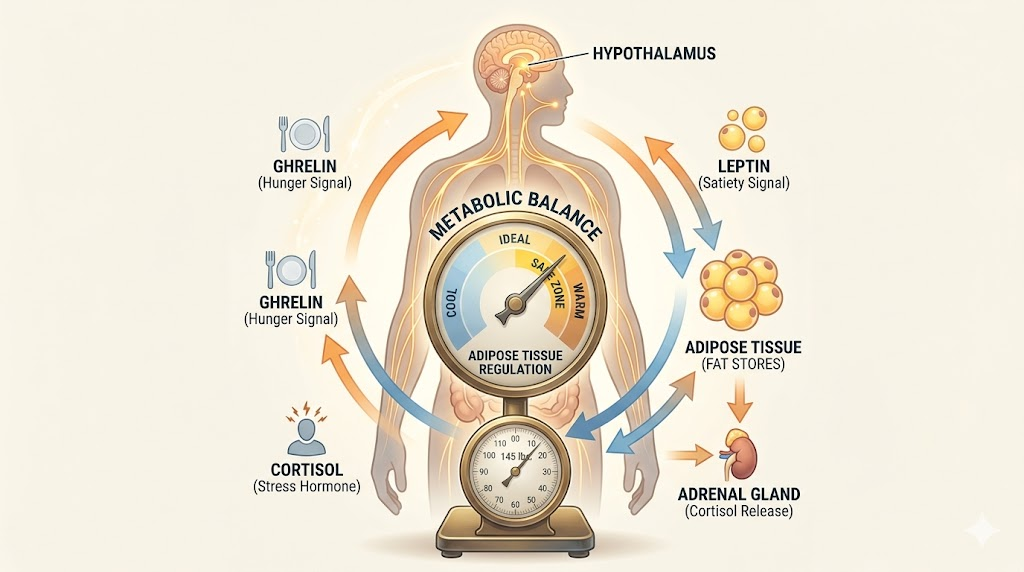
But Hormones are not the only factors. There are multiple other layers to your brain interpreting the set weight.
Firstly, your genes influence fat cell number, fat cell size, and how your hypothalamus responds to hunger signals.
Secondly, your adipose tissue history. If you had gained significant weight during childhood or adolescence, you have built more fat cells than someone who did not. The more fat you carry, the more leptin you produce, and the more your body considers the elevated leptin as your normal and drives overfeeding. In the cycle, Overfeeding will develop leptin resistance where the brain stops hearing the signal clearly and hence pushes the set point upward over time. More fat cells mean your body defends a higher set point.
Thirdly, the least identified factor is chronic stress or cortisol that drives visceral fat accumulation and alters hypothalamic sensitivity. Stress-related sleep deprivation also releases more ghrelin and suppresses leptin. Just two nights of short sleep can drive a 24 per cent increase in hunger.
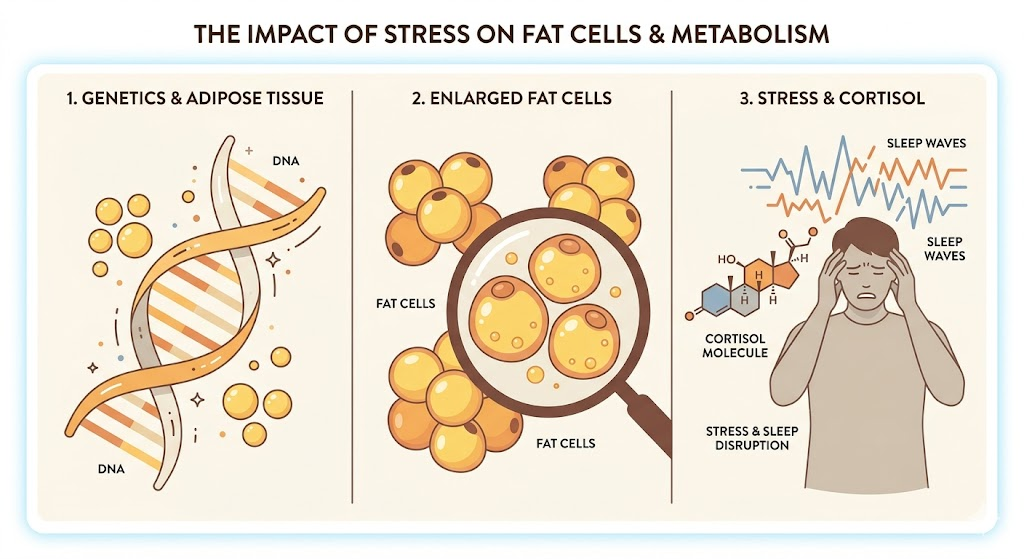
What Happens When You Drop Below the Set Point?
A Minnesota Starvation Experiment by Keys et al. in 1950 tested men who were reduced to roughly 75 per cent of their body weight. They became obsessed with food, lost the ability to concentrate on anything else, became emotionally volatile, and experienced severe metabolic slowdown. The relevant point is this: these were healthy, psychologically normal men before the study. Dropping below the set point triggered a physiological state that resembles semi-starvation, even if they were objectively not starving by any clinical measure. The semi-starvation state itself created the psychological symptoms.
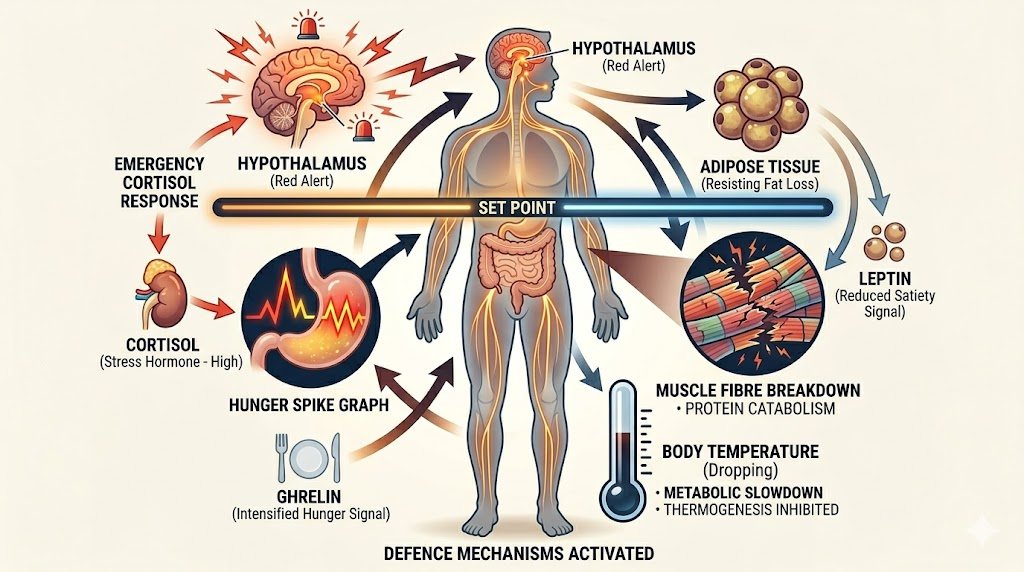
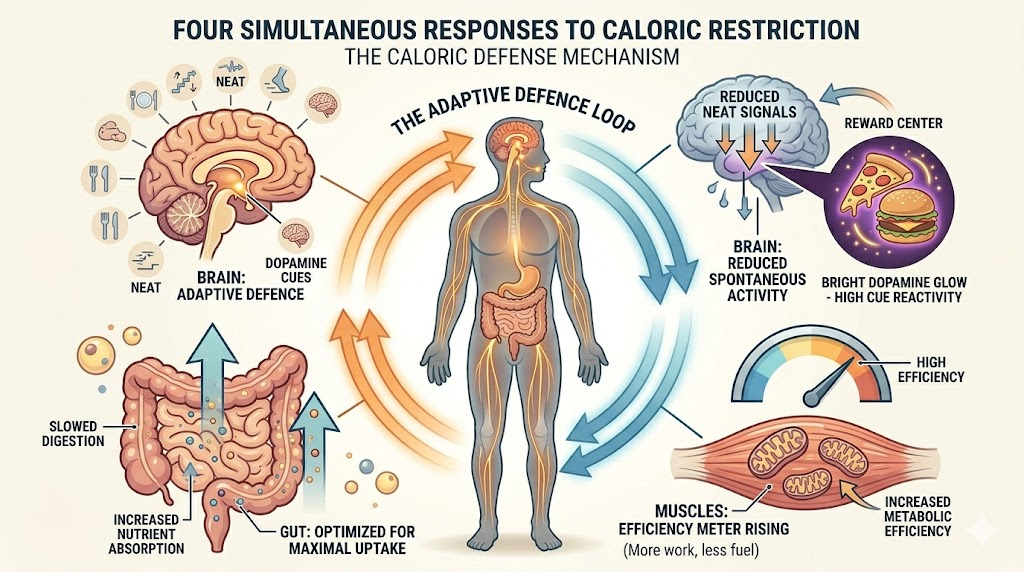
When you eat less, the body launches a coordinated, multi-system defence campaign.
Physically, your metabolic rate drops. Non-exercise activity thermogenesis (NEAT) also drops. NEAT is typically all movement that is not formal exercise, from picking or lifting regular objects, posture adjustments, taking stairs, general walking, to gesturing while talking. When you restrict calories, the brain unconsciously reduces NEAT. You sit more. You move less without realising it. The gut absorbs more nutrients per unit of food. Your intestines slow down the transit time because it aims to extract more calories from the same meal. Muscle burns fewer calories doing the same exercise you did before you lost weight.
Psychologically, the brain increases the reward value of food. Food looks better, smells stronger, and feels more rewarding. This is not a weakness. It is the brain up-regulating dopamine circuits to motivate eating. You are literally more vulnerable to food cues after dieting than before.
Hormonally, leptin crashes rapidly, even faster than fat mass falls. The brain interprets this as catastrophic energy depletion and activates starvation mode at the hypothalamus. Hunger becomes preoccupying. Sleep quality drops. Libido falls. The immune system weakens temporarily. Core body temperature drops slightly. Thyroid hormone output drops. This directly lowers metabolic rate across all tissues. You feel cold, sluggish, and mentally slower. Cortisol rises. The body treats being below the set point as a threat to survival. Elevated cortisol preserves blood glucose by breaking down muscle and drives fat storage preferentially in the abdominal region when eating resumes. The body begins preferentially breaking down muscle alongside fat, because muscle is metabolically expensive and the body wants to reduce its own energy requirements. This lean mass catabolism, and it makes regaining weight even easier afterwards, because you rebuild fat before you rebuild muscle.
The Rebound: Why the Weight Comes Back Heavier
The weight rebound after going below the set point is not a failure of discipline. It is the termination of a biological emergency response.
Once normal eating resumes, the body does not simply return to where it was. It overshoots the original set point slightly on rebound. If your set weight was 70 kg before you started losing weight, the next set weight might climb to around 75 kg. This fat overshoot is an evolutionary mechanism that is preparing for the next period of scarcity. Your body is essentially saying: “That set weight was dangerous. Let me store a little extra, just in case.” The unfortunate consequence is that your second attempt at weight loss becomes harder than the first. You are now defending a higher set point than you were before.
This blog is not meant to discourage you. It is meant to reframe the entire conversation around weight loss. The point is that all the crash diets, aggressive caloric restriction and huge mass loss in small periods work against your biology. Now let’s see what works?
Gradual, sustained changes.
Yes, slow and steady wins the race. If you reevaluate your weight loss journey and try to orient it more towards sustained weight management than rapid loss, you can recalibrate the set point downward over the years. Yes- years, not counted weeks. The goal is not to fight your body. The goal is to slowly renegotiate with it.
Working With Your Set Point, Not Against It
You have the answer now. There is no quick fix.
There is no supplement, no crash protocol, and no biohack that overrides a defended biological system built over millions of years of evolution. However, the set point is not a life sentence either. It is more like a thermostat with a dial that moves slowly when you apply the right consistent pressure over time. The goal is not to fight your biology. The goal is to renegotiate with it gradually enough that your body stops treating the change as a threat.
Before going to the solution, understand that the set point is not your enemy. It is simply a system doing its job based on the information it has been given over the years and decades. You can bring it down with sustained lifestyle changes maintained for one to three years.
Instead of asking “how fast can I lose this weight,” the more useful question becomes “what changes can I sustain indefinitely?”. A change that you can sustain for three years will shift your set point. You can maintain a lower and more harmonised set weight for the rest of your life without feeling like constantly fighting your body. Behaviours will gradually become default, hunger patterns will change, and food preferences will shift. Biologically, your hypothalamus will recalibrate to a new defended range because the new lifestyle and hormone levels will lower the “store more food” signal it was receiving.
1. Slow the Rate of Loss Deliberately
The single biggest mistake people make is losing weight too fast. Aggressive caloric deficits trigger the full defence cascade. Your body interprets rapid weight loss as a famine emergency, not a lifestyle choice. Research suggests that losses of roughly 0.5 to 1 per cent of body weight per week are slow enough that the hormonal alarm system does not fully activate. This is the concept of staying below the defence threshold. At this pace, leptin does not crash dramatically, ghrelin does not surge chronically, and the hypothalamus does not interpret the change as starvation. I know, this feels frustratingly slow. But that impatience is itself a psychological trap worth recognising. The faster you want to lose weight, the more you are working against the very system you need on your side.
2. Use Diet Breaks and Refeeds Strategically
A diet break is a planned period of two to four weeks where you return to maintenance calories after a stretch of deficit eating. A refeed is a shorter version. It is typically one to two days of eating at maintenance and then resuming a week of deficit phase.
Both strategies work. It temporarily restores leptin levels. When you eat at maintenance, leptin rises back toward its baseline, and the hypothalamus believes that no famine is occurring. Metabolic rate recovers partially too. When you return to a deficit after a break, the body responds less aggressively.
Please note that diet breaks are not cheating. They are not a loss of control. Yes, it stalls weight loss, and for a temporary period of time, the body will restore glycogen and water, which will lead to a weight spike. But remember, this is a temporary change. When you return to a deficit again (after that short break), you will lose the weight much faster and progress further with a recharged body.
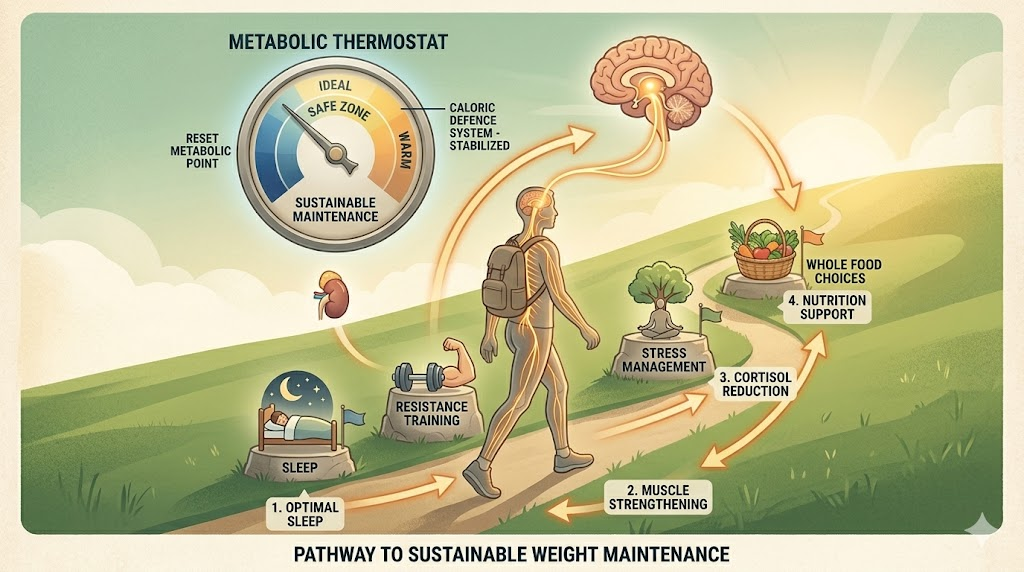
3. Prioritise Resistance Training, Protein and Fibre
Resistance training does something cardio cannot: it changes your body composition at the cellular level. Building lean muscle mass increases your resting metabolic rate because muscle tissue is metabolically expensive to maintain. Every kilogram of muscle you add raises the number of calories your body burns at rest. This gradually shifts the energy equation your hypothalamus is monitoring.
More importantly, resistance training appears to influence leptin sensitivity. When muscle cells become more metabolically active, the brain receives clearer energy sufficiency signals from leptin. This is the mechanism by which body recomposition, losing fat while maintaining or gaining muscle, can shift the set point downward without triggering the aggressive defence response that pure caloric restriction causes.
The practical implication is that the number on the scale matters less than your body composition ratio. Two people can weigh the same but have entirely different set point pressures depending on how much of that weight is muscle versus fat.
Protein is specifically important here. High protein intake suppresses ghrelin more effectively than carbohydrate or fat. It also preserves lean muscle mass during a caloric deficit, which protects metabolic rate. Research consistently shows that protein at roughly 1.6 to 2.2 grams per kilogram of body weight supports both muscle retention and appetite regulation during weight loss. Dietary fibre improves gut signalling to the hypothalamus through gut-brain axis communication. This is an emerging area of research, but the practical takeaway is that vegetables, legumes, and whole grains are not just calorie fillers. They are active participants in the hormonal conversation your gut has with your brain about how much energy you need.
4. Manage Chronic Stress as a Biological Priority
Most weight loss programmes ignore this entirely because it is harder to measure and sell than a meal plan. The mechanism worth understanding is this. When you are chronically stressed, your hypothalamus receives a continuous distress signal. It responds by defending a higher energy reserve because, in evolutionary terms, stress meant danger, and danger meant you might need fuel to survive or flee. Your body is storing fat for an emergency that is never coming, but it does not know that. Structured breathwork, regular low-intensity movement like walking, meaningful social connection, and time in natural environments are not soft wellness suggestions; they are direct interventions in the hormonal environment that governs your set point.
Further, stress affects sleep quality immensely. Poor sleep essentially simulates the hormonal state of being below your set point, even when you are not. You wake up hungrier, your brain is more responsive to food cues, and your capacity for impulse control is reduced. You are fighting hunger biology with a weakened decision-making system. That is a losing battle every time. Seven to nine hours of quality sleep per night is not a lifestyle luxury. It is the hormonal foundation on which every other weight management strategy rests.
And that’s it! That is all I know and can share at this point of time!

Leave a Reply